Cervical cancer is largely preventable through HPV vaccination and regular screening, as recommended by national guidelines, and it can be cured if detected early and treated promptly.
Cervical cancer is the fourth most common cancer in women globally with around 660,000 new cases and around 350,000 deaths in 2022. The highest rates of cervical cancer incidence and mortality are in low- and middle-income countries.
Cervical cancer is caused by persistent infection with human papillomavirus (HPV). Women living with HIV are 6 times more likely to develop cervical cancer compared to women without HIV.

New cases globally in 2022
Deaths globally in 2022
Most common cancer in women globally
Women living with HIV are 6 times more likely to develop cervical cancer
Almost all cases of cervical cancer are caused by infection with oncogenic types of human papillomavirus (HPV).
Human papillomavirus (HPV) is a common sexually transmitted infection which can affect the skin, genital area, anal area and throat. Almost all sexually active people will be infected at some point, usually without symptoms.
In most cases, the immune system clears the virus naturally. Persistent infection with certain carcinogenic types of HPV can cause abnormal cells that may develop into cancer.
It usually takes 15-20 years for abnormal cells to become cancer. In women with weakened immune systems, such as untreated HIV, this process can be faster and take 5-10 years.

Boosting public awareness, strengthening health literacy, and improving access to information and services are key to prevention and control across the life course:
For girls 9-14 years is highly effective at preventing infection, cervical cancer and other HPV-related cancers.
From age 30 (25 years in women living with HIV) can detect cervical precancer, and when coupled with timely treatment can prevent progression to cervical cancer.
At any age, early detection of women with symptoms, followed by prompt quality treatment, can cure cervical cancer.
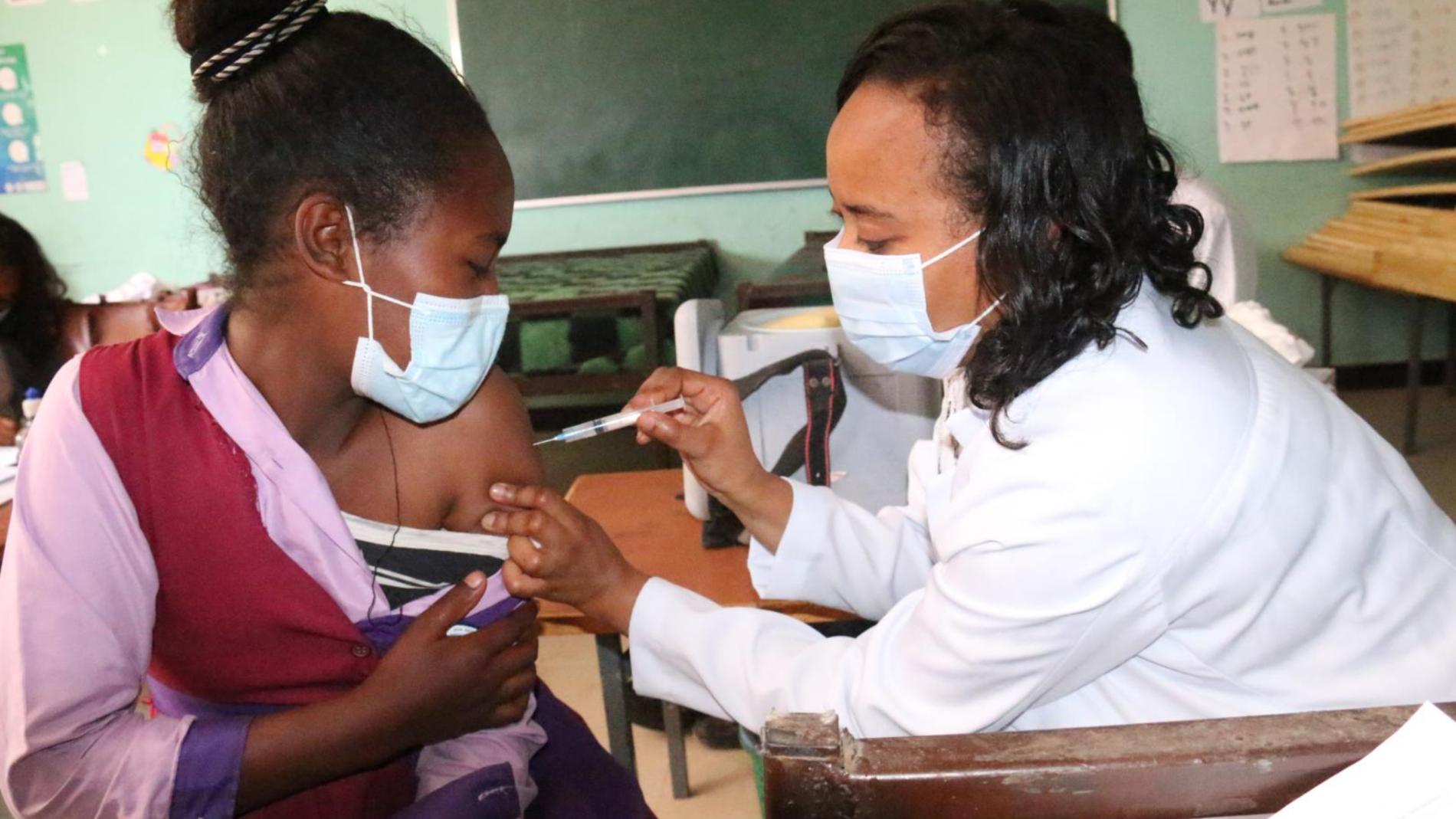
Women should be screened for cervical cancer with a high-performance test every 5-10 years starting at age 30. Women living with HIV should be screened every 3-5 years, starting at age 25.
The global strategy encourages a minimum of two lifetime screens with a high-performance test by age 35 and again by age 45. Precancers rarely cause symptoms, which is why regular cervical cancer screening is important, even if you have been vaccinated against HPV.

After a positive screen, a health-care provider can look for changes on the cervix (such as precancers) which may develop into cervical cancer if left untreated. Treatment of precancers is a simple and effective procedure to prevent cervical cancer.
Treatment of precancerous lesions is usually quick and may involve limited discomfort compared to other medical procedures. The process involves examining the cervix after applying acetic acid, with or without magnification, to locate the lesion and determine the appropriate treatment.

Women should consult a health-care professional if they notice:
Clinical evaluations and diagnostic tests are essential for confirming cervical cancer. These are generally followed by referral for treatment services.

Can include procedures to remove cancerous tissue, ranging from local excision to more extensive surgery depending on cancer stage.
Uses high-energy rays to kill cancer cells. Can be external or internal (brachytherapy).
Uses drugs to kill cancer cells, often used in combination with other treatments for advanced disease.
Provides supportive care and pain management to improve quality of life for patients with advanced cancer.
Management pathways for invasive cancer care are important to ensure that a patient is referred promptly and supported as they navigate the steps to diagnosis and treatment decisions. A multidisciplinary team should ensure diagnosis and staging takes place prior to treatment decisions.